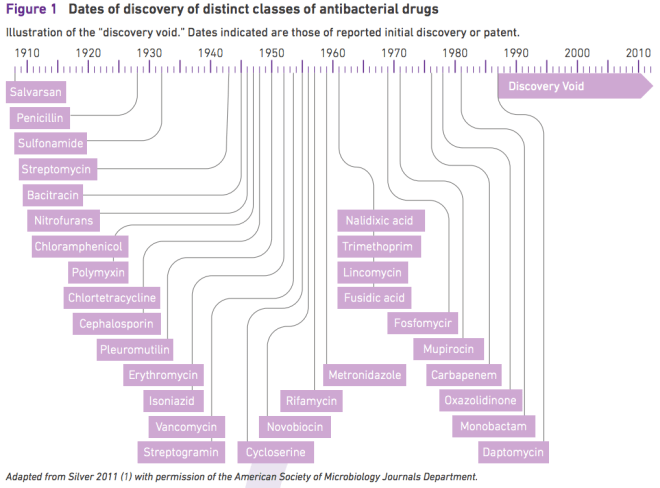
The World Health Organization has issued a lengthy report (pdf) rounding up the best available international data on drug-resistant bacteria and warning that the post-antibiotic era of our nightmares could be coming soon:
The WHO report, “Antimicrobial resistance: global report on surveillance”, collates data from 114 countries, looking at the seven most common bacteria responsible for serious disease and regional levels of resistance. … Avoiding the proliferation of antibiotics resistance should have been easy. WHO’s recommendations are, as ever, for people to use their prescriptions as instructed by their physician and to not share antibiotics. We know that not finishing a course of antibiotics can leave bacteria in the body and help it towards building a resistance. It should be avoidable. But there are other issues, such as overuse with livestock. In all cases, WHO is urging for “harmonised global standards”.
Another problem is that drug companies don’t put much effort into developing new antibiotics:
[R]esearch in this area has largely stalled, and only a handful of new antibiotics have been created over the past decade. That’s partly because it isn’t as profitable for pharmaceutical companies to invest in creating new drugs. Last year, the U.S. government formed a partnership with a pharma giant in the hopes of spurring innovation. Some infectious disease experts are urging Congress to pass tax credits to encourage the development of new antibiotics.
Susannah Locke reminds us why this is a really, really big problem:
It’s easy to forget what the world was like before the first antibiotic was discovered in 1928. Diseases like pneumonia and simple scrapes and infections could often cause death. Today, antibiotics have become indispensable for modern medicine — they’re used for surgeries, transplants, kidney dialysis. Without antibiotics, giving birth would be much more dangerous. Without antibiotics, an estimated one in six hip replacement patients would die.
The short story is that we really, really don’t want this to happen. You can read more about what the post-antibiotic world would look like in Maryn McKenna’s story here.
Russell Saunders, a pediatrician, can’t imagine “what it would be like to practice medicine without recourse to antibiotics”:
I get immensely frustrated when I encounter lazy medical providers who scribble out a prescription for a Z-Pak for every patient who smiles the right way. Even though I know it makes some people happy to leave my office with a script, I am professionally obligated to be parsimonious with a resource as precious as effective antibiotics. Hopefully, with increasing awareness of the antibiotic-resistance problem will come less pressure on providers to err on the side of treating disgruntled patients.